Introduction: Why Cloud Is Transforming U.S. Healthcare
Healthcare and life sciences in the United States are undergoing structural digital transformation. Hospitals, research labs, biotech firms, and pharmaceutical companies generate massive volumes of data—electronic health records (EHRs), imaging files, genomics datasets, wearable device streams, insurance claims, and clinical trial data.
Traditional on-premise infrastructure cannot efficiently process or scale such high-volume, high-velocity, and sensitive data. Cloud computing solves this challenge by offering scalable storage, high-performance computing, AI-powered analytics, and regulatory-compliant environments.
Major providers such as Amazon Web Services, Microsoft Azure, and Google Cloud offer HIPAA-eligible cloud services tailored for healthcare organizations.
Cloud in healthcare is not just about storage—it powers AI diagnostics, drug discovery, telemedicine platforms, population health analytics, and genomic sequencing.
1. Electronic Health Records (EHR) Hosting
Hospitals use cloud infrastructure to store and manage EHR systems securely. Instead of maintaining physical servers, patient data is hosted in encrypted cloud environments.
Real-world example: Large U.S. hospital networks migrate EHR systems to Azure cloud to enable multi-location access while maintaining compliance with HIPAA regulations.
Cloud ensures availability, disaster recovery, and secure access controls.
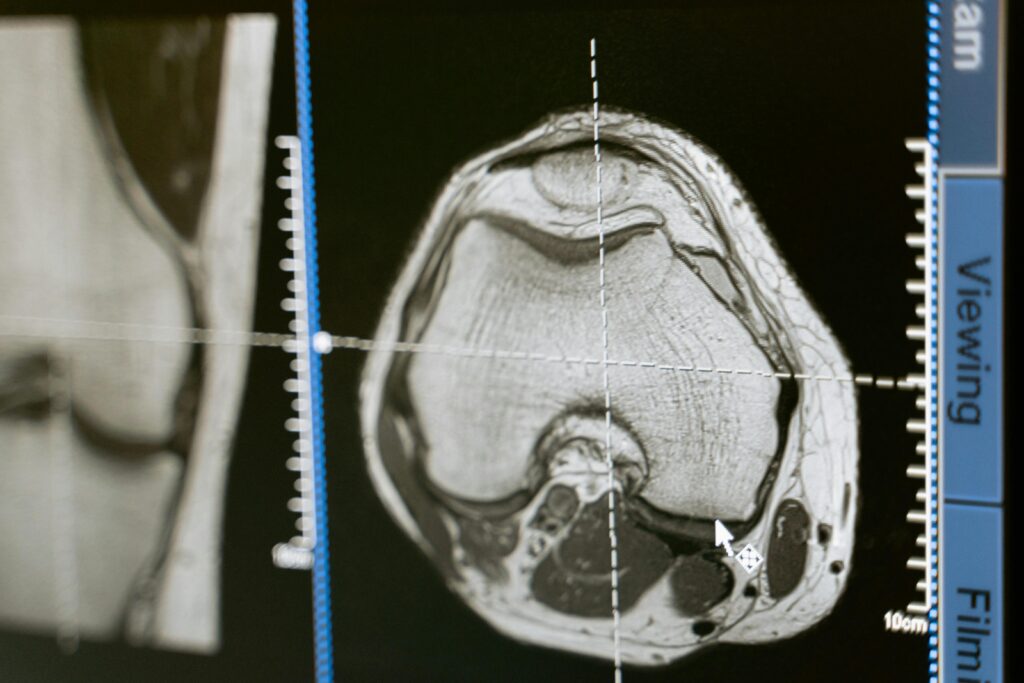
2. Medical Imaging & Radiology Data Management
Medical imaging files (MRI, CT scans, X-rays) require large storage capacity. Cloud enables scalable image archiving systems.
Example: Radiology departments store imaging data in AWS cloud storage, enabling physicians to access scans remotely for faster diagnosis.
This reduces latency in patient treatment.
3. AI-Powered Diagnostics
Cloud platforms provide GPU-based computing to train AI models for disease detection.
Example: AI systems analyze radiology images to detect early-stage cancer patterns using cloud-based machine learning tools.
This accelerates diagnosis and reduces human error.
4. Genomics & DNA Sequencing
Genomic sequencing generates terabytes of raw data. Cloud provides high-performance computing to process these datasets efficiently.
Example: Biotech firms use Google Cloud to analyze genome sequencing data during personalized medicine research.
Cloud shortens research timelines significantly.
5. Drug Discovery & Clinical Trials
Pharmaceutical companies use cloud computing to simulate molecular interactions and manage clinical trial data.
Example: Clinical trial platforms hosted in AWS enable real-time patient monitoring and data aggregation across multiple states.
Cloud improves trial efficiency and regulatory documentation.
6. Telemedicine & Remote Care Platforms
Telehealth applications require secure video streaming, patient scheduling, and prescription management.
Example: U.S. telemedicine providers use cloud infrastructure to scale during peak demand periods while ensuring encrypted consultations.
Cloud enables nationwide remote healthcare access.
7. Population Health Analytics
Healthcare providers analyze community-level health data to identify disease trends.
Example: Public health agencies process vaccination and outbreak data using cloud analytics dashboards.
Cloud enables faster decision-making during emergencies.
8. Internet of Medical Things (IoMT)
Connected medical devices generate real-time patient data streams.
Example: Wearable heart monitors send continuous data to cloud servers, allowing doctors to monitor patients remotely.
Cloud ensures scalable real-time processing.
9. Data Interoperability & Integration
Healthcare systems often operate across different platforms. Cloud enables API-based integration.
Example: Hospitals integrate lab systems, pharmacy systems, and billing systems via cloud-based middleware.
This improves workflow efficiency.
10. Security & HIPAA Compliance
Cloud providers offer encryption, audit logs, identity management, and compliance frameworks.
Example: Healthcare institutions use HIPAA-compliant cloud storage with role-based access control to secure patient records.
Security investments by cloud providers often exceed what small hospitals can afford independently.
11. Disaster Recovery & Business Continuity
Healthcare services must operate 24/7.
Cloud ensures automated backups and geographic redundancy.
Example: During natural disasters, hospitals continue accessing patient data through distributed cloud servers.
Operational resilience improves significantly.
12. Cost Optimization & Budget Control
Cloud converts large capital expenditures into predictable operational expenses.
Healthcare organizations avoid hardware procurement and maintenance costs.
Auto-scaling ensures resources are used efficiently.
13. Scalability for Research Institutions
Research labs require temporary high-performance computing for experiments.
Cloud allows them to scale compute resources during research phases and reduce usage afterward.
This flexibility enhances innovation without heavy infrastructure investment.
14. Real-Time Collaboration in Life Sciences
Cloud-based platforms allow researchers across states to collaborate on shared datasets securely.
Example: Multi-institution cancer research projects share anonymized datasets via secure cloud portals.
Collaboration accelerates medical breakthroughs.
15. Predictive Analytics & Preventive Healthcare
Cloud-based AI tools analyze historical patient data to predict disease risks.
Example: Predictive models identify high-risk diabetes patients, enabling early intervention programs.
Preventive care reduces long-term healthcare costs.
PROS OF CLOUD COMPUTING IN HEALTHCARE
1. Massive Scalability for Growing Medical Data
Healthcare data grows exponentially—EHR records, imaging scans, genomics, wearable device streams, and clinical trial datasets. Traditional data centers struggle to scale quickly without expensive hardware expansion.
Cloud platforms provide elastic storage and computing power. Hospitals can instantly scale up during flu season spikes or large research projects without purchasing new infrastructure.
Example: A multi-state hospital network using Amazon Web Services can increase storage capacity dynamically as patient records increase.
Scalability ensures healthcare providers never “run out of infrastructure.”
2. Faster AI & Diagnostic Innovation
Cloud platforms offer GPU-based computing necessary for AI training and medical imaging analysis. This allows healthcare organizations to deploy machine learning models without building expensive supercomputers.
Example: AI systems analyzing radiology images in cloud environments can detect abnormalities faster than manual review alone.
This improves diagnostic speed and potentially patient survival rates.
3. Cost Structure Optimization (CapEx to OpEx)
Healthcare institutions traditionally invest millions in data centers, servers, and IT maintenance.
Cloud shifts costs from capital expenditure (buying hardware) to operational expenditure (subscription-based usage). This improves financial predictability and budget flexibility.
Smaller clinics benefit significantly since they avoid high upfront infrastructure investments.
4. Enhanced Disaster Recovery & Business Continuity
Hospitals cannot afford downtime. Natural disasters, cyberattacks, or hardware failures can disrupt patient care.
Cloud providers distribute data across multiple geographic regions. If one data center fails, another automatically takes over.
This redundancy significantly reduces operational risk.
5. Improved Collaboration Across Institutions
Life sciences research often involves multiple institutions. Cloud enables secure, shared environments for data exchange.
Example: Genomic research teams across different states can collaborate in real time using shared cloud datasets hosted on Google Cloud.
This accelerates medical breakthroughs.
6. Stronger Cybersecurity Investments
Major cloud providers invest billions annually in cybersecurity—often more than individual hospitals can afford.
They offer encryption, identity access management, audit logging, threat detection, and compliance certifications.
While security still depends on proper configuration, enterprise-grade infrastructure enhances baseline protection.
7. Remote Patient Monitoring & Telehealth Enablement
Cloud supports real-time data transmission from wearable devices and telemedicine platforms.
Example: A heart monitor sends continuous patient data to cloud servers for physician review.
This improves chronic disease management and expands access to care in rural areas.
CONS OF CLOUD COMPUTING IN HEALTHCARE
1. Data Breach Risks & Misconfiguration
Healthcare data is extremely sensitive. While cloud platforms are secure by design, misconfigured access controls or weak identity management can expose patient information.
Human error remains a leading cause of cloud breaches.
A single breach can result in regulatory penalties and reputational damage.
2. Regulatory & Compliance Complexity
Healthcare organizations must comply with HIPAA and other federal/state regulations.
Cloud adoption requires proper Business Associate Agreements (BAAs), encryption protocols, audit trails, and documentation.
Compliance management adds administrative overhead.
3. Vendor Lock-In Risk
Migrating large healthcare systems to one provider can create dependency.
Switching providers later can be expensive and technically complex.
For example, institutions deeply integrated with Microsoft Azure services may face migration challenges if changing platforms.
Multi-cloud strategies help reduce this risk but increase complexity.
4. Ongoing Operational Costs
While cloud reduces upfront capital costs, subscription expenses can accumulate over time.
Poor cost governance can lead to budget overruns due to overprovisioned resources or unused compute instances.
Healthcare organizations must implement cost monitoring tools.
5. Internet Dependency
Cloud-based healthcare systems rely on stable internet connectivity.
Network outages can temporarily limit system access, especially in rural hospitals.
Hybrid systems may mitigate this risk but increase infrastructure complexity.
6. Data Migration Challenges
Migrating legacy healthcare systems to cloud environments is technically complex.
Historical data formats, integration with outdated applications, and downtime risks make migration projects resource-intensive.
Poor planning can disrupt patient services.
7. Cultural & Workforce Resistance
Healthcare IT teams accustomed to on-prem systems may resist cloud transformation.
Training and change management are essential to ensure smooth adoption.
Without internal expertise, cloud systems may be underutilized.
Conclusion: Data-Driven Healthcare Infrastructure
Cloud computing has become foundational to U.S. healthcare and life sciences. It enables AI-powered diagnostics, genomic research acceleration, telehealth expansion, secure patient data management, and predictive healthcare analytics.
As healthcare data continues to grow exponentially, cloud infrastructure ensures scalability, compliance, and computational power. Organizations that strategically adopt cloud with strong security governance will achieve operational efficiency, faster research outcomes, and improved patient care quality.
Cloud is not replacing healthcare expertise—it is enhancing it with intelligent infrastructure.
Frequently Asked Questions (FAQ)
1. Is cloud computing safe for patient data?
Yes, when configured properly under HIPAA compliance frameworks with encryption and access controls.
2. How does cloud improve patient care?
It enables faster diagnostics, remote monitoring, AI insights, and real-time collaboration among providers.
3. Is cloud cost-effective for hospitals?
It reduces capital infrastructure investment and allows flexible resource scaling.
4. Can small clinics use cloud solutions?
Yes. Many cloud providers offer scalable plans suitable for small practices.
5. What is the biggest challenge of cloud adoption in healthcare?
Data security management and regulatory compliance during migration.
For your reference